
Rare but preventable: know the signs of Toxic Shock Syndrome

The sudden onset of a high fever and other symptoms may call for a visit to the emergency room to rule out toxic shock syndrome. (U.S. Air Force photo by Airman Xiomara M. Martinez)
Years after Air Force Capt. Rebecca Lauters worked in an emergency room, the memory of a young woman who came in gravely ill still stands out. The patient was in her 20s, Lauters thought, with symptoms so severe that she was barely responsive. The diagnosis: toxic shock syndrome.
The National Institutes of Health defines toxic shock syndrome as a condition caused by a toxin that’s produced by some types of staphylococcus bacteria. When the toxins are released into the blood stream, they spread to the organs, which can lead to shock, illness, and, potentially, death.
“Toxic shock syndrome is not common, but we can possibly decrease the prevalence even more by making women aware of the signs and how they can prevent it,” said Lauters, a physician specializing in family medicine at Eglin Air Force Base in Florida.
Lauters said in 2016, the Centers for Disease Control and Prevention received reports of 323 cases of TSS in the United States among men and women. Of those cases, 26 were fatal, she said.
“Early symptoms are similar to other infections, but they can progress quickly to become life-threatening,” said Lauters. In such cases, she recommends seeking medical attention immediately. Symptoms include a sudden onset of fever greater than 102 degrees, a widespread red rash, nausea and vomiting, headache, muscle aches, abdominal pain, diarrhea, and/or disorientation.
She said women need to be aware of a particular warning sign: “If you’re at the onset of your period and you start feeling like this and have this rash, you need to be seen by a provider. The biggest reason for fatality is that toxic shock is not recognized soon enough.”
In women, TSS has been linked with tampon use during menstruation, with nearly half of current cases linked to tampon use, NIH said. Lauters said women ages 15-24 are at greater risk, most likely due to the lack of knowledge about proper tampon usage. Diagnoses of TSS spiked during the 1970s and 80s as a result of a substance in the tampons at the time, but the number has since declined and remained steady since the late 1980s, she said.
Army Lt. Col. Caela Miller, an obstetrician-gynecologist at Tripler Army Medical Center in Hawaii, and deputy consultant for obstetrics and gynecology to the Office of the Surgeon General, said the spike in infections caused companies producing feminine products to change how they made tampons.
“After that happened, the rate of TSS became very rare,” said Miller, adding that it’s unclear why some women develop it and others don’t. She recommends women use the lowest absorbency tampon possible and change them frequently, with no more than six to eight hours in between.
“You want to change it as frequently as possible, even on light flow days,” said Miller, who advises against wearing a tampon overnight. For women working in a field environment, symptoms of TSS are similar to those of heatstroke, she warned. “If you’re in an environment where it’s not possible to change tampons frequently, you may want to consider other options, such as pads or birth control that helps delay the menstrual cycle.”
Women can develop TSS from diaphragm and sponge usage as well, Miller said. According to the National Institutes of Health, TSS can also be associated with skin infections, burns, recent childbirth, recent surgery, and wound infection after surgery.
Once a person goes into shock, the likelihood of survival depends on how early antibiotics, fluids, and blood pressure supporting medications are received, said Miller.
“It’s a very difficult diagnosis to make, and I think it’s something that’s hard because tampons are sort of just a fact of life in developed countries,” said Miller. She recommends going to a facility that has intensive care unit capabilities. Recovery can range from a couple of days to a couple of weeks, depending on the severity and stage of illness.
Miller warned that women who have developed TSS are more likely to have recurrent infections. After the initial infection, the vagina can become colonized with the staphylococcus bacteria that produces the toxin, so if a woman has survived TSS, she should no longer use tampons, she said.
While the possibility of TSS shouldn’t prevent women from wearing tampons, it’s important to be aware of the symptoms and seek medical attention if they arise, especially during the first few days of the menstrual cycle, said Miller.
“Most women who wear tampons are just fine, but it’s important to realize that occasionally, complications like toxic shock syndrome can happen,” said Miller.
Women and Depression
Article
10/30/2018

1 in every 8 women develops clinical depression during her lifetime
Women's health remains priority for doctors turned medical museum volunteers
Article
10/25/2018

The Handwerkers clearly enjoy volunteerism
Military Midwives Advance Medicine
Video
10/23/2018

Military midwives assist in advancing military medicine. Capt. Brittany Hannigan uses educational opportunities to bring evidence-based practices to the patient's bedside.
‘Strong progress’ in decreasing death from breast cancer
Article
10/23/2018

Improvements in detection, treatment pave the way
Women’s Health: Taking time for yourself
Article
10/16/2018
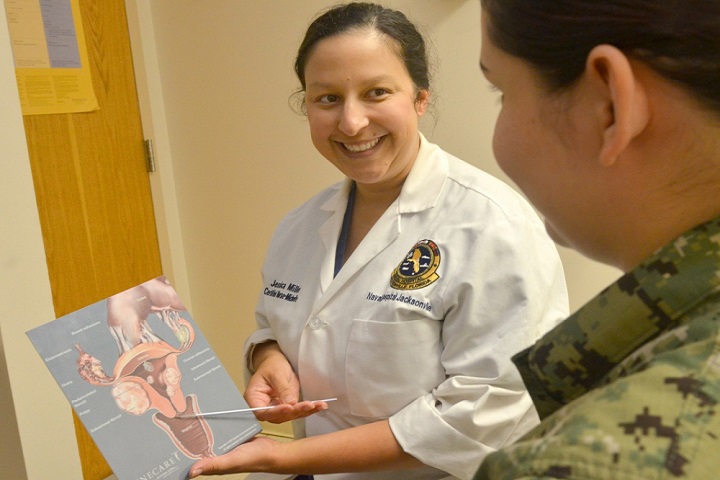
The top two causes of death for women are heart disease and cancer
Military midwives as educators
Video
10/15/2018

Within the military, midwives serve as educators. Kwuan Paruchabutr shares how midwives ensure that all medical staff are well trained in women's health care.
Sticks and stones can break bones – and so can osteoporosis
Article
10/11/2018

Steps to take today to build a future of healthy bones
Military Midwives in Leadership Roles
Video
10/5/2018

The duties of certified nurse midwives go far beyond the labor delivery room. Cmdr. Kim Shaughnessy explains how midwives hold leadership positions across the Military Health System and how they help shape women's health policy.
Mammograms recommended for early detection of breast cancer
Article
10/4/2018
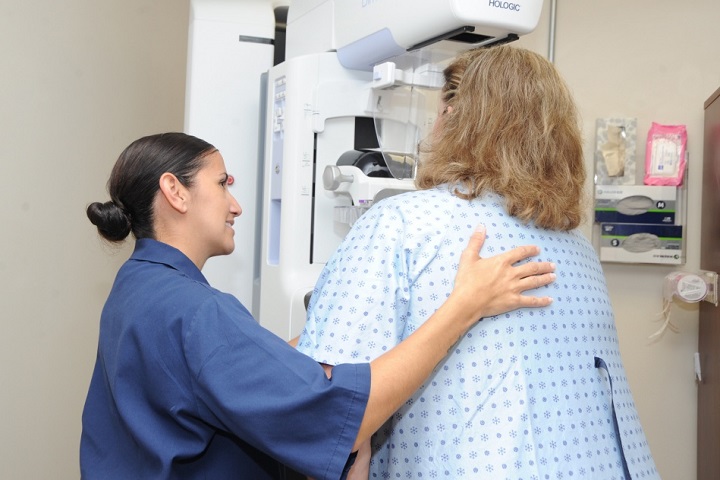
A mammogram is a low-dose x-ray used to detect the early stages of breast cancer
Midwives in the Military
Video
10/3/2018

Military midwives are key in the Department of Defense's priority of medical readiness. Army Lt. Col. Danielle Molinar shares ways midwives keep female soldiers ready to deploy.
New simulator preps WBAMC staff for OB emergencies
Article
5/1/2018
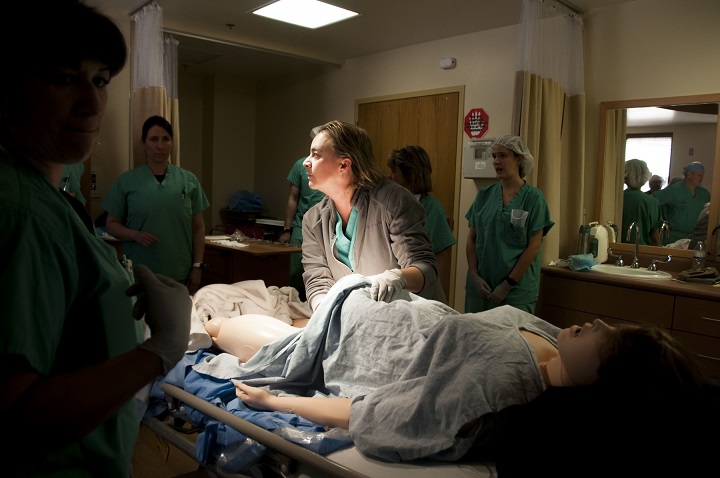
The state-of-the-art simulator provides medical staff up to various cutting-edge training scenarios
Getting tested for STIs is an 'important part of sexual health'
Article
4/26/2018

Chlamydia and gonorrhea are two of the most common sexually transmitted infections in the United States. Taking preventive steps, like getting tested and practicing safe sex, can help reduce risk of infection or spreading the infection to others.
Fort Belvoir corpsman comes through for moms
Article
4/20/2018

Striving to empower, lactation consultants critical for mothers, babies
The fight against cervical cancer
Article
1/24/2018

Learn about two weapons that can stop this cancer in its tracks
January is Cervical Cancer Awareness Month
Article
1/18/2018

Cervical cancer deaths have decreased by more than 50 percent due to regular screening tests that detect abnormalities before cancer develops





















.png)












No hay comentarios:
Publicar un comentario