
Cervical ectropion
The cervix is the lowest and tightly closed tubular part of the uterus or womb. It is lined with columnar epithelium on the inside of the tubular canal, while the part that faces downwards, and extends into the birth canal, is lined by squamous epithelium.
When columnar epithelium grows downwards onto this outward-facing portion of the cervix, which is called the ectocervix, it is called cervical ectropion or erosive cervicitis.
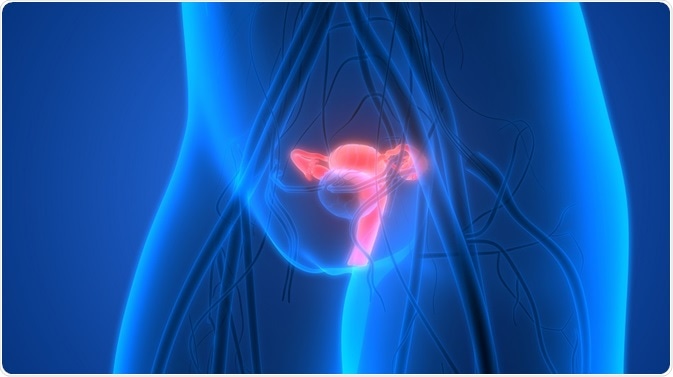 Credit: Magic mine/ Shutterstock.com
Credit: Magic mine/ Shutterstock.comCauses
Columnar epithelium is normally found in the endocervix in very young women, but during and after puberty the process of metaplasia transforms this epithelium into stratified squamous epithelium. In some cases, columnar epithelium may persist in some areas and these are called cervical erosions or cervical ectropion.
The exact etiology of cervical ectropion is unknown, but many factors are suspected to play a role. They include:
- Pregnancy
- Adolescence-related changes
- Oral contraceptives, whether combined or progesterone-only
Many clinicians think that cervical ectropion is a symptom of chronic cervical inflammation, or chronic cervicitis. Others think that it is not a disease condition at all but merely a variant of normal physiology.
The issue is confused by the fact that many women with ectropion also have symptoms such as increased vaginal discharge, pelvic pain, spotting after sexual intercourse, recurrent attacks of cervical inflammation, or pain during coitus. Though this may be a coincidence, it is the cause of much dispute as to the precise clinical significance of ectropion.
Desquamative inflammatory vaginitis (DIV) is a condition in which a woman has painful intercourse, a feeling of vaginal irritation and profuse yellowish discharge from the vagina, which contains many neutrophils and parabasal cells shed from the deeper layers of the vaginal epithelium. The discharge is quite acidic.
The cause is suspected to be due to infection by anerobic bacteria or trichomonas infection. It could also be due to lichen planus, atrophic vaginitis, estrogen deficiency, Staphylococcal infection or some unknown immune phenomenon. It is sometimes seen in association with cervical ectropion. Epidemiologic studies show that chlamydial infection and perhaps HIV infection is more frequent in women with cervical ectopy.
Diagnosis
Diagnosis of cervical ectropion is usually made following a colposcopic examination, using a magnifier to obtain images of the cervix which can be stored digitally and compared both with other images and with earlier pictures of the same cervix, to assess progression of the lesions over time or following treatment. This is superior to subjective assessment with the naked eye.
Treatment
Cervical erosions are treated differently in different regions of the world, depending on the clinical significance ascribed to their presence. Thus, in many Third World countries, symptoms related to the reproductive tract are often thought to be due to the erosions which are considered a form of chronic cervicitis. For this reason, they are treated in a variety of ways. These include:
- Cryotherapy (freezing the columnar epithelium by the local application of liquid nitrogen)
- Electrocoagulation (where the erosions are destroyed by passing electric current through them)
- Local application of DNA
- Microwave coagulation of the tissues
- Laser ablation
- Interferon-alpha application in the form of suppositories
It is important to realize that none of the trials conducted so far have answered the question of whether cervical ectropion should be treated in the first place, and if so, the endpoint of treatment should be. In most trials the improvement of the appearance of the cervix was taken as evidence of the success of the treatment, rather than the extent of relief of symptoms.
It was not known what percentage of women with erosions had symptoms such as mucopurulent discharge, or postcoital bleeding. In developed nations, cervical ectropion is thought to be a normal variant and no treatment is prescribed.
Reviewed by Afsaneh Khetrapal Bsc (Hons)
Last Updated: Feb 16, 2018
























.png)










No hay comentarios:
Publicar un comentario