Current Cigarette Smoking Among Adults — United States, 2005–2015 | MMWR |
| MMWR Weekly Vol. 65, No. 44 November 11, 2016 |
| PDF of this issue |
Current Cigarette Smoking Among Adults — United States, 2005–2015
Weekly / November 11, 2016 / 65(44);1205–1211
Ahmed Jamal, MBBS1; Brian A. King, PhD1; Linda J. Neff, PhD1; Jennifer Whitmill, MPH1; Stephen D. Babb, MPH1; Corinne M. Graffunder, DrPH1(View author affiliations)
Summary
What is already known about this topic?
Tobacco use is the leading cause of preventable disease and death in the United States, and cigarettes are the most commonly used tobacco product among U.S. adults.
What is added by this report?
The proportion of U.S. adults who smoke cigarettes declined from 20.9% in 2005 (45.1 million smokers) to 15.1% in 2015 (36.5 million smokers), and the proportion of daily smokers declined from 16.9% to 11.4%. However, disparities in cigarette smoking persist; for example, in 2015, cigarette smoking prevalence was higher among persons who have serious psychological distress (40.6%) than among persons without serious psychological distress (14.0%).
What are the implications for public health practice?
Proven population-based interventions, including tobacco price increases, comprehensive smoke-free laws, anti-tobacco mass media campaigns, and barrier-free access to tobacco cessation counseling and medications, are critical to reducing cigarette smoking and smoking-related disease and death among U.S. adults, particularly among subpopulations with the highest smoking prevalence.
Ahmed Jamal, MBBS1; Brian A. King, PhD1; Linda J. Neff, PhD1; Jennifer Whitmill, MPH1; Stephen D. Babb, MPH1; Corinne M. Graffunder, DrPH1(View author affiliations)
Tobacco use is the leading cause of preventable disease and death in the United States, and cigarettes are the most commonly used tobacco product among U.S. adults (1,2). To assess progress toward achieving the Healthy People 2020 target of reducing the proportion of U.S. adults who smoke cigarettes to ≤12.0% (objective TU1.1),* CDC assessed the most recent national estimates of cigarette smoking prevalence among adults aged ≥18 years using data from the 2015 National Health Interview Survey (NHIS). The proportion of U.S. adults who smoke cigarettes declined from 20.9% in 2005 to 15.1% in 2015, and the proportion of daily smokers declined from 16.9% to 11.4%. However, disparities in cigarette smoking persist. In 2015, prevalence of cigarette smoking was higher among adults who were male; were aged 25–44 years; were American Indian/Alaska Native; had a General Education Development certificate (GED); lived below the federal poverty level; lived in the Midwest; were insured through Medicaid or were uninsured; had a disability/limitation; were lesbian, gay, or bisexual; or who had serious psychological distress. Proven population-based interventions, including tobacco price increases, comprehensive smoke-free laws, anti-tobacco mass media campaigns, and barrier-free access to tobacco cessation counseling and medications, are critical to reducing cigarette smoking and smoking-related disease and death among U.S. adults, particularly among subpopulations with the highest smoking prevalences (3).
NHIS is an annual, nationally representative, in-person survey of the noninstitutionalized U.S. civilian population. The NHIS sample adult core questionnaire is administered to a randomly selected (sample) adult in the household, and, in 2015, included 33,672 adults aged ≥18 years; the response rate was 55.2%. Current cigarette smokers were adults who smoked ≥100 cigarettes during their lifetime and, at the time of interview, reported smoking every day or on some days.
Data were weighted to adjust for differences in the probabilities of selection and nonresponse, and to provide nationally representative estimates. Current smoking was assessed overall and by sex, age, race/ethnicity, education, poverty status,† U.S. region,§ health insurance coverage at the time of survey,¶ disability/limitation status,** sexual orientation,†† and serious psychological distress status§§. Two different measures for psychological distress were assessed (e.g., a dichotomous (yes/no) measure for serious psychological distress, and a four-category (no, low, moderate, or high) measure for the degree of psychological distress.¶¶ The mean number of cigarettes smoked per day was calculated among daily smokers. Differences between groups were assessed using a Wald test, with statistical significance defined as p< 0.05. Logistic regression was used to assess linear trends using annual NHIS data from 2005–2015. Relative percentage changes in prevalence rates during 2005–2015 were calculated.***
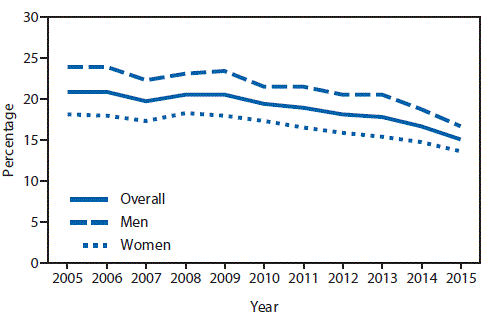
Current cigarette smoking among U.S. adults declined from 20.9% (an estimated 45.1 million adults) in 2005 to 15.1% (36.5 million) in 2015, a 27.7% decline (p for trend < 0.05) (Figure 1). During 2005–2015, significant declines in smoking prevalence were observed among all subgroups by sex, poverty status, and U.S. region (p< 0.05) (Table).
Current cigarette smoking was significantly lower in 2015 (15.1%) than in 2014 (16.8%) (p< 0.05); however, there were differences in smoking prevalence by sex, age group, race/ethnicity, educational attainment, economic status, U.S. region, insurance and disability status, sexual orientation, and serious psychological distress status. In 2015, current cigarette smoking prevalence was higher among males (16.7%) than females (13.6%) and among adults aged 25–44 years (17.7%) than those aged ≥65 years (8.4%). Prevalence was highest among American Indian/Alaska Natives (21.9%) and was more than three times the prevalence among non-Hispanic Asians, who had the lowest prevalence (7.0%). Among adults aged ≥25 years, prevalences ranged from a high of 34.1% among persons with a GED to a low of 3.6% among persons with a graduate degree. Prevalence among persons living below the poverty level (26.1%) was nearly twice that of persons at or above this level (13.9%). By region, the highest prevalence was in the Midwest (18.7%) and lowest was in the West (12.4%). Smoking prevalence was higher among Medicaid enrollees (27.8%) and uninsured persons (27.4%) than among persons covered by private health insurance (11.1%) or by Medicare only (8.9%), and higher among adults with a disability/limitation (21.5%) than among adults reporting no disability/limitation (13.8%). In addition, reported smoking prevalence was higher among adults who were lesbian, gay, or bisexual (20.6%) than heterosexual adults (14.9%). In 2015, persons with serious psychological distress reported a higher smoking prevalence (40.6%) than did persons without serious psychological distress (14.0%) (Table). Among adults with high psychological distress, prevalence was highest among persons aged 25–44 years (44.3%) and lowest among persons aged ≥ 65 years (18.9%) (Figure 2).
Among current smokers during 2005–2015, the number of daily smokers decreased from 36.5 million (80.8%) to 27.6 million (75.7%), while the number who smoked on some days increased from 8.7 million (19.2%) to 8.9 million (24.3%) (p for trend < 0.05). Among daily smokers, the mean number of cigarettes smoked per day declined from 16.7 in 2005 to 14.2 in 2015 (p for trend < 0.05), but did not change significantly between 2014 (13.8 per day) and 2015 (14.2 per day). Moreover, despite an increase in the proportion of daily smokers who smoked 1–9 cigarettes per day since 2012, this proportion did not change significantly between 2014 (26.9%) and 2015 (25.1%). Similarly, during 2014–2015, no significant change occurred in the proportion of daily smokers who smoked 20–29 cigarettes per day (27.4% to 29.3%) or ≥30 cigarettes per day (6.9% to 6.8%) (Figure 3).
Discussion
During 2005–2015, the prevalence of cigarette smoking among U.S. adults declined from 20.9% to 15.1%, including a 1.7 percentage point reduction during 2014–2015 alone, indicating progress toward achieving the Healthy People 2020 goal of reducing cigarette smoking prevalence to ≤12.0%. However, 36.5 million U.S. adults currently smoke cigarettes, and disparities in smoking prevalence persist. Cigarette smoking prevalence was higher among adults who are male; younger; American Indian/Alaska Native; have less education; live below the federal poverty level; live in the Midwest or South; are insured through Medicaid or are uninsured; have a disability/limitation; are lesbian, gay, or bisexual; or have serious psychological distress. Moreover, after declines during previous years, the mean number of cigarettes smoked per day among daily smokers did not change significantly from 2014 to 2015. The Surgeon General has concluded that the burden of death and disease from tobacco use in the United States is overwhelmingly caused by cigarettes and other combusted tobacco products (1). Accordingly, enhanced and sustained implementation of proven population-level interventions, including tobacco price increases, anti-tobacco mass media campaigns, comprehensive smoke-free laws, and enhanced access to help in quitting tobacco use, are critical to reducing smoking-related disease and death in the United States (3).
Efforts to address the disparities noted in this report are crucial to further reducing smoking prevalence in the United States (1). Differences in smoking by race/ethnicity might be partly explained by sociocultural influences, and disparities by education might be partly attributable to variations in the understanding of the range of health hazards caused by smoking (4,5). Differences by health insurance coverage might be partly attributable to variations in tobacco cessation coverage and access to evidence-based cessation treatments across insurance types (6). Consistent with previous research, smoking prevalence was higher among persons with high or serious psychological distress (7,8), which could be partly explained by higher levels of addiction and dependence, lack of financial resources, less access to cessation treatments, and stressful living conditions among these persons (7,8). Many smokers with behavioral health problems would like to quit and are able to quit with assistance (8,9). Assessing the smoking status of all patients served in psychiatric inpatient and outpatient settings, and integrating evidence-based cessation interventions such as counseling and medications into mental health treatment plans could help reduce smoking prevalence in this population (7,8).
The findings in this report are subject to at least four limitations. First, smoking status was self-reported and was not validated by biochemical testing; however, self-reported smoking status correlates highly with serum cotinine levels (10). Second, because NHIS does not include institutionalized populations and persons in the military, results are not generalizable to these groups. Third, the NHIS response rate of 55.2% might have resulted in nonresponse bias. Finally, these estimates might differ from those in other surveys. These differences can be partially explained by varying survey methodologies, types of surveys administered, and definitions of current smoking; however, trends in prevalence are comparable across surveys (1).
Sustained comprehensive state tobacco control programs funded at CDC-recommended levels could accelerate progress in reducing adult smoking prevalence and smoking-related disease, death, and economic costs (3). However, during 2016, despite combined revenues of $25.8 billion from settlement payments and tobacco taxes in all states, state spending on tobacco control programs is projected to be $468 million (1.8% of revenues),††† representing < 15% of the CDC-recommended level of funding for all states combined (3). Implementation of comprehensive tobacco control interventions can result in substantial reductions in tobacco-related disease and death and billions of dollars in savings from averted medical costs (1). In particular, the health care system offers important opportunities to reduce smoking, especially for vulnerable populations, by implementing system changes to make tobacco dependence treatment a standard of care and by working with health insurers to cover evidence-based cessation treatments with minimal barriers and to promote their use (3,6).
Corresponding author: Ahmed Jamal, ajamal@cdc.gov, 770-488-5493.
1Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC.
† Based on reported family income: 2005 estimates are based on reported family income and 2004 poverty thresholds published by the U.S. Census Bureau, and 2015 estimates are based on reported family income and 2014 poverty thresholds published by the U.S. Census Bureau.
§ Northeast: Connecticut, Maine, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Vermont. Midwest: Illinois, Indiana, Iowa, Kansas, Michigan, Minnesota, Missouri, Nebraska, North Dakota, Ohio, South Dakota, and Wisconsin. South: Alabama, Arkansas, Delaware, District of Columbia, Florida, Georgia, Kentucky, Louisiana, Maryland, Mississippi, North Carolina, Oklahoma, South Carolina, Tennessee, Texas, Virginia, and West Virginia. West: Alaska, Arizona, California, Colorado, Hawaii, Idaho, Montana, Nevada, New Mexico, Oregon, Utah, Washington, and Wyoming.
¶ Private coverage: includes adults who had any comprehensive private insurance plan (including health maintenance organizations and preferred provider organizations). Medicaid: for adults aged < 65 years, includes adults who do not have private coverage, but who have Medicaid or other state-sponsored health plans including Children’s Health Insurance Program (CHIP); for adults aged ≥65 years, includes adults aged ≥65 years who do not have any private coverage but have Medicare and Medicaid or other state-sponsored health plans including CHIP; Medicare only: includes adults aged ≥65 years who only have Medicare coverage; Other coverage: includes adults who do not have private insurance, Medicaid, or other public coverage, but who have any type of military coverage, coverage from other government programs, or Medicare. Uninsured: includes adults who have not indicated that they are covered at the time of the interview under private health insurance, Medicare, Medicaid, CHIP, a state-sponsored health plan, other government programs, or military coverage.
** Disability/limitation was defined based on self-reported presence of selected impairments including vision, hearing, cognition, and movement. Limitations in performing activities of daily living was defined based on response to the question, “Does [person] have difficulty dressing or bathing?” Limitations in performing instrumental activities of daily living defined based on response to the question, “Because of a physical, mental, or emotional condition, does [person] have difficulty doing errands alone such as visiting a doctor’s office or shopping?” Any disability/limitation was defined as a “yes” response pertaining to at least one of the disabilities/limitations listed (e.g., vision, hearing, cognition, movement, activities of daily living, or instrumental activities of daily living). A random sample of half the respondents from the 2015 Person File were asked about disability/limitation.
†† Starting in 2013, sexual orientation questions were added to NHIS for the first time. To determine sexual orientation, adult respondents were asked, “Which of the following best represents how you think of yourself?” with a response options of: “gay” (“lesbian or gay” for female respondents), “heterosexual,” that is, “not gay” (“not lesbian or gay” for female respondents), “bisexual,” “something else,” and “I don’t know the answer.”
§§ The six-question Kessler (K6) scale was developed to identify persons with a high likelihood of having a diagnosable mental illness and associated functional limitations. The K6 scale asked how often during the past 30 days the respondents felt a) “so sad that nothing could cheer them up”; b) “nervous”; c) “restless or fidgety”; d) “hopeless”; e) “that everything was an effort”; or f) “worthless.” Responses were on a five-point Likert scale ranging from none of the time to all of the time. For each question, a value of zero, one, two, three, or four was assigned to the response: “none of the time,” “a little of the time,” “some of the time,” “most of the time,” or “all of the time,” respectively. Responses to the six items were summed to yield a K6 score of 0–24, with higher scores indicating greater psychological distress. Additional information available at https://www.cdc.gov/nchs/data/databriefs/db203.pdf.
¶¶ Based on K6 scale, the degree of psychological distress is presented as a four-category measure with no psychological distress (score = 0), low psychological distress (score = 1–5), moderate psychological distress (score = 6–10), and high psychological distress (score = 11–24) (http://www.samhsa.gov/data/sites/default/files/CBHSQ-DR-C11-MI-Mortality-2014/CBHSQ-DR-C11-MI-Mortality-2014.pdf).
*** [(2005 estimate - 2015 estimate)/2005 estimate] x 100.
References
- US Department of Health and Human Services. The health consequences of smoking—50 years of progress: a report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, CDC; 2014. http://www.surgeongeneral.gov/library/reports/50-years-of-progress/full-report.pdf
- Hu SS, Neff L, Agaku IT, et al. Tobacco product use among adults—United States, 2013–2014. MMWR Morb Mortal Wkly Rep 2016;65:685–91. CrossRef PubMed
- CDC. Best practices for comprehensive tobacco control programs—2014. Atlanta, GA: US Department of Health and Human Services, CDC; 2016. http://www.cdc.gov/tobacco/stateandcommunity/best_practices/index.htm
- Siahpush M, McNeill A, Hammond D, Fong GT. Socioeconomic and country variations in knowledge of health risks of tobacco smoking and toxic constituents of smoke: results from the 2002 International Tobacco Control (ITC) Four Country Survey. Tob Control 2006;15(Suppl 3):iii65–70. CrossRef PubMed
- Pampel FC, Krueger PM, Denney JT. Socioeconomic disparities in health behaviors. Annu Rev Sociol 2010;36:349–70. CrossRef PubMed
- McAfee T, Babb S, McNabb S, Fiore MC. Helping smokers quit—opportunities created by the Affordable Care Act. N Engl J Med 2015;372:5–7. CrossRef PubMed
- American Legacy Foundation. A hidden epidemic: tobacco use and mental illness. Washington, DC: American Legacy Foundation; 2011.
- Gfroerer J, Dube SR, King BA, et al. . Vital signs: current cigarette smoking among adults aged ≥18 years with mental illness—United States, 2009–2011. MMWR Morb Mortal Wkly Rep 2013;62:81–7. PubMed
- Schroeder SA, Morris CD. Confronting a neglected epidemic: tobacco cessation for persons with mental illnesses and substance abuse problems. Annu Rev Public Health 2010;31:297–314, 1p, 314. CrossRef PubMed
- Binnie V, McHugh S, Macpherson L, Borland B, Moir K, Malik K. The validation of self-reported smoking status by analysing cotinine levels in stimulated and unstimulated saliva, serum and urine. Oral Dis 2004;10:287–93. CrossRef PubMed























.png)












No hay comentarios:
Publicar un comentario