Zika and Birth Defects: The Evidence Mounts
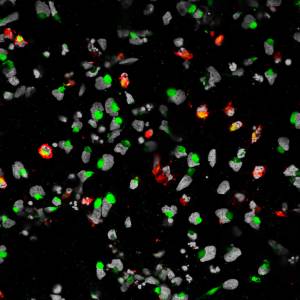
Caption: Human neural progenitor cells (gray) infected with Zika virus (green) increased the enzyme caspase-3 (red), suggesting increased cell death.
Credit: Sarah C. Ogden, Florida State University, Tallahassee
Credit: Sarah C. Ogden, Florida State University, Tallahassee
Recently, public health officials have raised major concerns over the disturbing spread of the mosquito-borne Zika virus among people living in and traveling to many parts of Central and South America [1]. While the symptoms of Zika infection are typically mild, grave concerns have arisen about its potential impact during pregnancy. The concerns stem from the unusual number of births of children with microcephaly, a very serious condition characterized by a small head and damaged brain, coinciding with the spread of Zika virus. Now, two new studies strengthen the connection between Zika and an array of birth defects, including, but not limited to, microcephaly.
In the first study, NIH-funded laboratory researchers show that Zika virus can infect and kill human neural progenitor cells [2]. Those progenitor cells give rise to the cerebral cortex, a portion of the brain often affected in children with microcephaly. The second study, involving a small cohort of women diagnosed with Zika virus during their pregnancies in Rio de Janeiro, Brazil, suggests that the attack rate is disturbingly high, and microcephaly is just one of many risks to the developing fetus. [3]
The NIH-supported study, described in a recent issue of Cell Stem Cell, was led by Guo-li Ming and Hongjun Song of Johns Hopkins University School of Medicine, Baltimore, and Hengli Tang of Florida State University, Tallahassee. Their research teams turned to human induced pluripotent stem (iPS) cells, derived from skin biopsies, to produce human neural progenitor cells (hNPCs). These cells are readily found in the developing brain and are capable of becoming neurons in the cerebral cortex.
The researchers found that Zika virus could readily infect those neural progenitors in lab dishes. In fact, within three days of inoculation, the virus had infected 65 to 90 percent of the cells. The infection also led to a 30 percent reduction in viable hNPCs, as some cells died and others grew more slowly. In another important experiment, the group discovered that, once infected, a neural progenitor cell turns into “a virus factory.” In other words, the virus exploits the cell’s own machinery to produce and release more Zika to infect more cells.
While these findings will need to be confirmed in clinical studies, they suggest for the first time that Zika virus can directly target these essential neural cells. They also help to explain how Zika infection could cause harm to the developing brain, providing a possible link to microcephaly.
Unfortunately, it now appears that microcephaly isn’t the only cause for worry about children exposed to Zika virus in the womb. In the second study, reported recently in The New England Journal of Medicine, a team of U.S. and Brazilian researchers enrolled 88 healthy pregnant Brazilian women who within the past five days had developed a red skin rash, one of the symptoms associated with Zika infection. Seventy-two of these women were later confirmed by blood and/or urine tests to have Zika virus, and 42 of those agreed to undergo an abdominal ultrasound.
Of the Zika-infected women, almost a third had developing babies that showed signs of very serious abnormalities by ultrasound. Five babies showed growth restrictions with or without microcephaly. Seven had other abnormalities of the central nervous system. Seven babies showed abnormally low levels of amniotic fluid or blood flow to the brain or umbilical cord. Doctors delivered one of the babies by emergency C-section due to a dangerous lack of amniotic fluid. Two babies in the study were stillborn just weeks before their due dates. None of the 16 Zika-uninfected women had pregnancies with fetal abnormalities.
These preliminary findings suggest that exposure to Zika virus is risky at any stage of pregnancy—even for developing babies that don’t appear to have microcephaly or other malformations. Further research is urgently needed, and these researchers have now enrolled a total of 280 Brazilian women into their ongoing study. They’ll also continue to follow the outcomes for these women and their children over the coming months.
Taken together, these studies strengthen the case that the Zika virus may well be behind the deeply troubling rise in microcephaly in Brazil. These new developments raise the question of why the ability of Zika virus to cause birth defects wasn’t previously known—after all, this virus has been around for a long time (it was originally described in 1947 in the Zika forest in Uganda). One possibility is that in endemic areas nearly all individuals are infected as children, have a mild illness, and then develop lifelong immunity. Only in the situation where a previously unexposed population encounters the virus in adulthood is the risk of active infection in pregnancy, and subsequent birth defects in the offspring, possible. (Scholars of virology will recognize this phenomenon as having similarities to rubella, or “German measles.”) The NIH is now working aggressively to develop a vaccine. But there are still many steps in development and testing before a vaccine could be made available to vulnerable populations. Meanwhile, CDC recommendations for travelers should be scrutinized by everyone.
References:
[1] Zika virus disease in the United States, 2015-2016. Centers for Disease Control and Prevention. 2016 Mar 9.
[2] Zika virus infects human cortical neural progenitors and attenuates their growth. Tang H, Hammack C, Ogden SC, Wen Z, Qian X, Li Y, Yao B, Shin J, Zhang F, Lee EM, Christian KM, Didier RA, Jin P, Song H, Ming G. Cell Stem Cell. 2016 Mar 4. [Epub ahead of print]
[3] Zika Virus Infection in Pregnant Women in Rio de Janeiro – Preliminary Report. Brasil P, Pereira JP Jr, Raja Gabaglia C, Damasceno L, Wakimoto M, Ribeiro Nogueira RM, Carvalho de Sequeira P, Machado Siqueira A, Abreu de Carvalho LM, Cotrim da Cunha D, Calvet GA, Neves ES, Moreira ME, Rodrigues Baião AE, Nassar de Carvalho PR, Janzen C, Valderramos SG, Cherry JD, Bispo de Filippis AM, Nielsen-Saines K. N Engl J Med. 2016 Mar 4. [Epub ahead of print]
Links:
Zika Virus (National Institute of Allergy and Infectious Diseases/NIH)
Microcephaly Information Page (National Institute of Neurological Disorders and Stroke/NIH)
Hongjun Song (Johns Hopkins University, Baltimore)
Hengli Tang (Florida State University, Tallahassee)
NIH Support: National Institute of Allergy and Infectious Diseases; National Institute of Neurological Disorders and Stroke





















.png)












No hay comentarios:
Publicar un comentario