 |
| MMWR Recommendations and Reports Vol. 65, No. RR-6 November 11, 2016 |
Core Elements of Outpatient Antibiotic Stewardship
Recommendations and Reports / November 11, 2016 / 65(6);1–12
Guillermo V. Sanchez, MPH, MSHS1; Katherine E. Fleming-Dutra, MD1; Rebecca M. Roberts, MS1; Lauri A. Hicks, DO1 (View author affiliations)
View suggested citationSummary
The Core Elements of Outpatient Antibiotic Stewardship provides a framework for antibiotic stewardship for outpatient clinicians and facilities that routinely provide antibiotic treatment. This report augments existing guidance for other clinical settings. In 2014 and 2015, respectively, CDC released the Core Elements of Hospital Antibiotic Stewardship Programs and the Core Elements of Antibiotic Stewardship for Nursing Homes. Antibiotic stewardship is the effort to measure and improve how antibiotics are prescribed by clinicians and used by patients. Improving antibiotic prescribing involves implementing effective strategies to modify prescribing practices to align them with evidence-based recommendations for diagnosis and management. The four core elements of outpatient antibiotic stewardship are commitment, action for policy and practice, tracking and reporting, and education and expertise. Outpatient clinicians and facility leaders can commit to improving antibiotic prescribing and take action by implementing at least one policy or practice aimed at improving antibiotic prescribing practices. Clinicians and leaders of outpatient clinics and health care systems can track antibiotic prescribing practices and regularly report these data back to clinicians. Clinicians can provide educational resources to patients and families on appropriate antibiotic use. Finally, leaders of outpatient clinics and health systems can provide clinicians with education aimed at improving antibiotic prescribing and with access to persons with expertise in antibiotic stewardship. Establishing effective antibiotic stewardship interventions can protect patients and improve clinical outcomes in outpatient health care settings.
Introduction
Antibiotic resistance is among the greatest public health threats today, leading to an estimated 2 million infections and 23,000 deaths per year in the United States (1). Although antibiotics are life-saving drugs that are critical to modern medicine, infections with pathogens resistant to first-line antibiotics can require treatment with alternative antibiotics that can be expensive and toxic. Antibiotic-resistant infections can lead to increased health care costs and, most importantly, to increased morbidity and mortality (1). The most important modifiable risk factor for antibiotic resistance is inappropriate prescribing of antibiotics. Approximately half of outpatient antibiotic prescribing in humans might be inappropriate, including antibiotic selection, dosing, or duration, in addition to unnecessary antibiotic prescribing (2–4). At least 30% of outpatient antibiotic prescriptions in the United States are unnecessary (5).
Antibiotic stewardship is the effort to measure antibiotic prescribing; to improve antibiotic prescribing by clinicians and use by patients so that antibiotics are only prescribed and used when needed; to minimize misdiagnoses or delayed diagnoses leading to underuse of antibiotics; and to ensure that the right drug, dose, and duration are selected when an antibiotic is needed (1,6). Antibiotic stewardship can be used in all health care settings in which antibiotics are prescribed and remains a cornerstone of efforts aimed at improving antibiotic-related patient safety and slowing the spread of antibiotic resistance. The goal of antibiotic stewardship is to maximize the benefit of antibiotic treatment while minimizing harm both to individual persons and to communities.
Background
Improving antibiotic prescribing in all health care settings is critical to combating antibiotic-resistant bacteria (7). Approximately 60% of U.S. antibiotic expenditures for humans are related to care received in outpatient settings (8). In other developed countries, approximately 80%–90% of antibiotic use occurs among outpatients (9,10). During 2013 in the United States, approximately 269 million antibiotic prescriptions were dispensed from outpatient pharmacies (11). Approximately 20% of pediatric visits (12) and 10% of adult visits (3) in outpatient settings result in an antibiotic prescription. Complications from antibiotics range from common side effects such as rashes and diarrhea to less common adverse events such as severe allergic reactions (13). These adverse drug events lead to an estimated 143,000 emergency department visits annually and contribute to excess use of health care resources (13). Antibiotic treatment is the most important risk factor for Clostridium difficile infection (14). In 2011, an estimated 453,000 cases of C. difficile infection occurred in the United States, approximately one third of which were community-associated infections (i.e., occurred in patients with no recent overnight stay in a health care facility) (15). As much as 35% of adult and 70% of pediatric C. difficile infections are community associated (15,16). One study estimated that a 10% reduction in overall outpatient antibiotic prescribing could reduce community-associated C. difficile infections by 17% (17). By reducing unnecessary antibiotic prescribing (18–20), antibiotic stewardship can prevent avoidable adverse events resulting from antibiotics.
In 2014 and 2015, respectively, CDC released the Core Elements of Hospital Antibiotic Stewardship Programs (21,22) and the Core Elements of Antibiotic Stewardship for Nursing Homes (23). This 2016 report, Core Elements of Outpatient Antibiotic Stewardship, provides guidance for antibiotic stewardship in outpatient settings and is applicable to any entity interested in improving outpatient antibiotic prescribing and use. The intended audiences for this guidance include clinicians (e.g., physicians, dentists, nurse practitioners, and physician assistants) and clinic leaders in primary care, medical and surgical specialties, emergency departments, retail health and urgent care settings, and dentistry, as well as community pharmacists, other health care professionals, hospital clinics, outpatient facilities, and health care systems involved in outpatient care (Box 1).
Leaders of organizations of any size and within any medical specialty, from single-provider clinics to large health care systems, are encouraged to commit to optimizing antibiotic prescribing and patient safety; implement at least one action in the form of a policy or practice to improve antibiotic prescribing; track and regularly report antibiotic prescribing practices to clinicians or enable clinician self-assessment on antibiotic prescribing; educate clinicians and patients on appropriate antibiotic prescribing; and ensure access to expertise on antibiotic prescribing. Before implementing antibiotic stewardship interventions, clinicians and outpatient clinic and health system leaders can identify opportunities to improve antibiotic prescribing. These opportunities include identifying high-priority conditions for intervention, identifying barriers that lead to deviation from best practices, and establishing standards for antibiotic prescribing based on evidence-based diagnostic criteria and treatment recommendations (Box 2). High-priority conditions are conditions for which clinicians commonly deviate from best practices for antibiotic prescribing and include conditions for which antibiotics are overprescribed, underprescribed, or misprescribed with the wrong antibiotic agent, dose, or duration. Barriers to prescribing antibiotics appropriately might include clinician knowledge gaps about best practices and clinical practice guidelines, clinician perception of patient expectations for antibiotics, perceived pressure to see patients quickly, or clinician concerns about decreased patient satisfaction with clinical visits when antibiotics are not prescribed. Standards for antibiotic prescribing can be based on national clinical practice guidelines by national health care professional societies such as the American Academy of Pediatrics, the American College of Physicians, or the Infectious Diseases Society of America or, if applicable, can be based on facility- or system-specific clinical practice guidelines. A summary of current national clinical practice guidelines for common outpatient infections in children and adults is available at http://www.cdc.gov/getsmart/community/for-hcp/outpatient-hcp/index.html.
Clinicians and clinic leaders can collaborate with relevant partners in the broader health care community to facilitate outpatient antibiotic stewardship (Box 3). To improve antibiotic prescribing, clinic leaders can implement effective strategies to modify prescribing behaviors and align them with evidence-based recommendations for diagnosis and management (1). Clinicians can expect outpatient antibiotic stewardship to improve the quality of patient care, slow the development of community antibiotic resistance, and reduce avoidable adverse drug events caused by unnecessary use of antibiotics (24,25).
Methods
CDC’s Core Elements of Outpatient Antibiotic Stewardship were developed through a combination of consolidating evidence-based antibiotic stewardship practices and building on or adapting known best practices for antibiotic stewardship across other clinical settings, such as the core elements outlined for hospitals (21,22) and nursing homes (23). A narrative review of evidence on outpatient antibiotic stewardship interventions, policies, and practices through May 2016 was conducted. A systematic review was not conducted because at least five systematic reviews on outpatient stewardship interventions have been performed since 2005 (24–28), of which the two most recent were published in 2015 and 2016 (24,25). The narrative review included the five systematic reviews (24–28), articles found through in-text citations, and new articles from a supplemental search of articles published during October 2015–May 2016. Information from selected citations included in the systematic reviews also was considered if it had not been specified previously in the systematic review. The supplemental search of PubMed identified English-language articles only published during October 2015–May 2016 with the following search terms: “antibiotic stewardship” or “antibiotic prescribing” or “antibiotic prescriptions” or “antimicrobial stewardship” or (“antibiotic” and “stewardship”) or (“antimicrobial” and “stewardship”). Articles identified through these methods were prioritized and included on the basis of relevance to outpatient antibiotic stewardship, defined as having 1) clearly stated study objectives to identify factors affecting outpatient antibiotic prescribing or to assess one or more outpatient antibiotic stewardship interventions, 2) been performed in outpatient settings similar to those common in the United States (e.g., study settings in which patients access antibiotics through prescriptions written by a clinician), 3) effectively reported outcomes related to antibiotic stewardship, 4) enrolled subjects with outpatient infections common in the United States, or 5) been previously cited as archetypal studies for stewardship interventions (http://www.cdc.gov/getsmart/community/improving-prescribing/interventions/index.html); included studies are available online at https://stacks.cdc.gov/view/cdc/41536). When no peer-reviewed evidence was available, expert opinion was substituted.
CDC identified subject-matter experts in outpatient antibiotic stewardship research, implementation, policy, and practice on the basis of peer-reviewed publications with representation from important outpatient specialties. Subject-matter experts were identified with expertise in pediatrics, internal medicine, family medicine, emergency medicine, infectious diseases, and pharmacy. CDC provided eight subject-matter experts with a draft of the core elements in April 2016. Subject-matter experts were asked for specific feedback on the feasibility, acceptability, recommended supplementary materials, and potential for the core elements to promote effective and meaningful improvements in outpatient antibiotic prescribing. In addition to written feedback via electronic correspondence, a 1-hour group teleconference was offered to all subject-matter experts, during which verbal feedback from each person was collected. CDC revised and refined the core elements using individual feedback received from the subject-matter experts.
Core Elements of Outpatient Antibiotic Stewardship
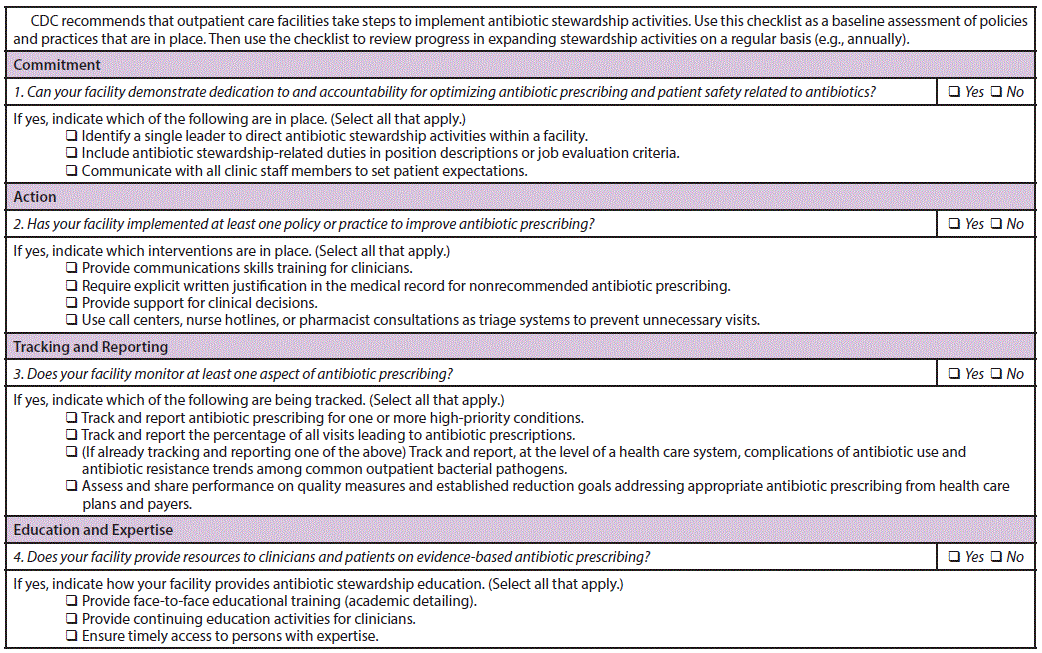
The Core Elements of Outpatient Antibiotic Stewardship follow and are summarized in a clinician checklist (Figure 1) and a facility checklist (Figure 2):
- Commitment: Demonstrate dedication to and accountability for optimizing antibiotic prescribing and patient safety.
- Action for policy and practice: Implement at least one policy or practice to improve antibiotic prescribing, assess whether it is working, and modify as needed.
- Tracking and reporting: Monitor antibiotic prescribing practices and offer regular feedback to clinicians, or have clinicians assess their own antibiotic prescribing practices themselves.
- Education and expertise: Provide educational resources to clinicians and patients on antibiotic prescribing, and ensure access to needed expertise on optimizing antibiotic prescribing.
Commitment
A commitment from all health care team members to prescribe antibiotics appropriately and engage in antibiotic stewardship is critical to improving antibiotic prescribing. Every person involved in patient care, whether directly or indirectly, can act as an antibiotic steward. Each clinician can make the choice to be an effective antibiotic steward during each patient encounter.
Clinicians can demonstrate commitment to appropriate antibiotic prescribing by doing the following:
- Write and display public commitments in support of antibiotic stewardship. For example, inappropriate antibiotic prescriptions for acute respiratory infections were reduced after clinicians displayed, in their examination rooms, a poster showing a letter from the clinician to their patients committing to prescribing antibiotics appropriately (18). This approach also might facilitate patient communication about appropriate antibiotic use.
Outpatient clinic and health care system leaders can commit to promoting appropriate antibiotic prescribing by doing any of the following:
- Identify a single leader to direct antibiotic stewardship activities within a facility. Appointing a single leader who is accountable to senior facility leaders is recommended for hospital stewardship programs (21,22), and this approach also might be beneficial in outpatient settings.
- Include antibiotic stewardship-related duties in position descriptions or job evaluation criteria. These duties can be listed for medical directors, nursing leadership positions, and practice management personnel and will help ensure staff members have sufficient time and resources to devote to stewardship. Although evidence in the outpatient settings is lacking, this type of leadership support has been shown to be important for hospital antibiotic stewardship programs (29).
- Communicate with all clinic staff members to set patient expectations. Patient visits for acute illnesses might or might not result in an antibiotic prescription. All staff members in outpatient facilities, including administrative staff members, medical assistants, nurses, allied health professionals, and medical directors, can improve antibiotic prescribing by using consistent messages when communicating with patients about the indications for antibiotics.
Action for Policy and Practice
Outpatient clinicians and clinic leaders can implement policies and interventions to promote appropriate antibiotic prescribing practices. A stepwise approach with achievable goals can facilitate policy and practice changes and help clinicians and staff members from feeling overwhelmed. As with all quality improvement efforts, assessment and modification of implemented policies and interventions are critical to improving antibiotic prescribing practices. Prioritizing interventions according to feasibility, acceptability, resource commitment, and anticipated barriers to change is important. Action is necessary to transform policy and practice into measurable outcomes.
Clinicians can implement at least one of the following actions to improve antibiotic prescribing:
- Use evidence-based diagnostic criteria and treatment recommendations. When possible, these criteria and recommendations should be based on national or local clinical practice guidelines informed by local pathogen susceptibilities. This can be accomplished by adhering to recommendations from clinical practice guidelines for common infections published by national professional societies such as the American Academy of Pediatrics and the Infectious Diseases Society of America (30–35).
- Use delayed prescribing practices or watchful waiting, when appropriate. Delayed prescribing can be used for patients with conditions that usually resolve without treatment but who can benefit from antibiotics if the conditions do not improve (e.g., acute uncomplicated sinusitis or mild acute otitis media). Clinicians can apply delayed prescribing practices by giving the patient or parent a postdated prescription and providing instructions to fill the prescription after a predetermined period or by instructing the patient to call or return to collect a prescription if symptoms worsen or do not improve (36–40). Watchful waiting means providing symptomatic relief with a clear plan for follow-up if infection symptoms worsen or do not improve. Watchful waiting and delayed antibiotic prescriptions are evidence-based approaches that can safely decrease antibiotic use when used in accordance with clinical practice guidelines (41–44).
Outpatient clinic and health care system leaders can take at least one of the following actions to improve antibiotic prescribing based on established standards or national clinical practice guidelines:
- Provide communications skills training for clinicians. Communications skills training can be used to promote strategies to address patient concerns regarding prognosis, benefits, and harms of antibiotic treatment; management of self-limiting conditions; and clinician concerns regarding managing patient expectations for antibiotics during a clinical visit (45,46).
- Require explicit written justification in the medical record for nonrecommended antibiotic prescribing. This technique has reduced inappropriate prescribing by holding clinicians accountable in the medical record for their decisions (19).
- Provide support for clinical decisions. Clinical decision support, which provides specific information in electronic or print form during the typical workflow, can facilitate accurate diagnoses and effective management of common conditions (e.g., discouraging antibiotic prescribing for acute bronchitis in healthy adults) (47–52).
- Use call centers, nurse hotlines, or pharmacist consultations as triage systems to prevent unnecessary visits. These resources can be used to reduce unnecessary visits for conditions that do not require a clinic visit (53), such as a common cold.
Tracking and Reporting
Tracking and reporting clinician antibiotic prescribing, also called audit and feedback, can guide changes in practice and be used to assess progress in improving antibiotic prescribing. When setting up tracking and reporting systems, decisions need to be made about the level at which to track and report (i.e., at the individual clinician level or at the facility level), which outcomes to track and report, and how to obtain the data for tracking and reporting. Sources of data might include automatic electronic medical record extraction, manual periodic chart reviews, or performance data on existing quality measures related to outpatient antibiotic prescribing (e.g., Healthcare Effectiveness Data and Information Set [HEDIS] measures). Analysis can occur at the individual clinician level or at the facility level (i.e., aggregate of all clinician antibiotic prescriptions). The preferred approach, when possible, is to track antibiotic prescribing at the individual clinician level. Individualized feedback provided to clinicians on antibiotic prescribing is an effective way to promote adherence to evidence-based guidelines (20,54–56). Effective feedback interventions have included comparison of clinicians’ performance with that of their peers (20), particularly with peers who perform in the top 10% on quality measures or in adherence to evidence-based guidelines (i.e., top-performing peers) (19). In turn, feedback from clinicians about stewardship interventions can help guide modifications to maximize the impact and improve the acceptability of stewardship interventions (57). In addition, a study that informed certain clinicians that they prescribed more antibiotics than 80% of their peers also resulted in reductions in overall antibiotic prescribing (58).
Tracking and reporting for identified high-priority conditions can be used to assess whether an antibiotic was appropriate for the assigned diagnosis, whether the diagnostic criteria were met before assigning an antibiotic-appropriate diagnosis, whether the selected antibiotic was the recommended agent, and whether the dose and duration were correct. Outpatient clinicians and clinic or health care system leaders can select outcomes to track and report on the basis of identified opportunities for improvement in their practice or clinics. Systems can track high-priority conditions identified as opportunities to improve clinician adherence to best practices and clinical practice guidelines for antibiotic prescribing (Box 2). For example, acute bronchitis is a common condition for which antibiotics are not recommended in national clinical practice guidelines, yet antibiotics are commonly prescribed (59,60). Therefore, leaders might choose to provide feedback on the percentage of acute bronchitis visits in which a clinician prescribed an antibiotic and include comparisons with their peers’ prescribing percentages for acute bronchitis. This paired tracking and reporting approach for selected high-priority conditions has reduced inappropriate antibiotic prescribing and improved antibiotic selection (19,20).
Systems also can track the percentage of visits for which an individual clinician prescribes antibiotics (e.g., number of all antibiotics prescribed for all diagnoses by a clinician divided by the total number of visits for all diagnoses for that clinician). Providing clinicians with these individualized percentages in comparison with their peers has reduced antibiotic prescribing (58) and can help minimize the influence of differences in clinicians’ diagnostic coding practices. A practice known as diagnosis shifting occurs when a clinician manipulates a diagnostic code to justify prescribing an antibiotic; for example, a clinician might record the code for pneumonia (which requires an antibiotic) when a patient has acute bronchitis (which does not require an antibiotic). Diagnosis shifting can be missed when tracking and reporting only one high-priority condition (e.g., only acute bronchitis), whereas tracking the percentage of all visits leading to antibiotic prescriptions is not affected by diagnosis shifting. However, when comparing metrics for antibiotic stewardship, the comparability of the clinicians’ patient populations should be considered because clinicians might treat patients with different underlying needs for antibiotics (e.g., a clinician who cares for a higher percentage of patients with immunosuppression than other clinicians in their clinic).
Certain health care systems also might be able to track and report the complications of antibiotic use (e.g., C. difficile infections, drug interactions, and adverse drug events) and antibiotic resistance trends among common outpatient bacterial pathogens (24). At the individual or clinic level, smaller sample sizes might make these measures less reliable or useful. In these cases, investigating C. difficile infections to assess for possible links to previous ambulatory care visits and antibiotic prescriptions might be used as a marker for possible adverse drug events.
Both clinicians and clinic leaders can be involved in antibiotic stewardship. Clinicians can track and report their own antibiotic prescribing practices by doing at least one of the following:
- Self-evaluate antibiotic prescribing practices. Clinicians can use self-evaluations to align their antibiotic prescribing practices with updated evidence-based recommendations and clinical practice guidelines.
- Participate in continuing medical education and quality improvement activities to track and improve antibiotic prescribing. Activities can be tailored by clinical specialty if conducted through health professional organizations and also might be used to meet licensure and other education and quality improvement requirements.
Outpatient clinic or health care system leaders can do at least one of the following:
- Implement at least one antibiotic prescribing tracking and reporting system. Outcomes to be tracked can include high-priority conditions that have been identified as opportunities for improvement in that clinic, the percentage of all visits leading to antibiotic prescriptions, and, for health systems, complications of antibiotic use and antibiotic resistance trends (if antibiotic prescribing outcomes are already being tracked). Outcomes can be tracked and reported by individual clinicians (which is preferred) and by facilities.
- Assess and share performance on quality measures and established reduction goals addressing appropriate antibiotic prescribing from health care plans and payers. The National Strategy for Combating Antibiotic-Resistant Bacteria aims to reduce inappropriate antibiotic use by 50% for monitored conditions in outpatient settings by 2020 (61). Current HEDIS measures include quality measures for appropriate testing for children with pharyngitis, appropriate treatment for children with upper respiratory infections (i.e., avoidance of antibiotics), and avoidance of antibiotic treatment in adults with acute bronchitis (62).
Education and Expertise
Education on appropriate antibiotic use can involve patients and clinicians. Education for patients and family members can improve health literacy and augment efforts to improve antibiotic use. Education for clinicians and clinic staff members can reinforce appropriate antibiotic prescribing and improve the quality of care (56,63,64). Deficits in clinician knowledge are seldom the only barrier to prescribing antibiotics appropriately in the outpatient setting. Effective clinician education often includes reviewing guidelines for appropriate antibiotic prescribing while also addressing the psychosocial pressures that influence antibiotic prescribing practices of clinicians (e.g., clinicians’ concerns about patient satisfaction). Access to colleagues and consultants with expertise (e.g., pharmacists and specialists) also is a valuable resource for improving antibiotic prescribing.
Clinicians can educate patients and families about appropriate antibiotic use by doing at least one of the following:
- Use effective communications strategies to educate patients about when antibiotics are and are not needed. For example, patients should be informed that antibiotic treatment for viral infections provides no benefit and thus should not be used for viral infections. Patients also should be informed that certain bacterial infections (e.g., mild ear and sinus infections) might improve without antibiotics. Explanations of when antibiotics are not needed can be combined with recommendations for symptom management; this combination of messages has been associated with visit satisfaction (65). In addition, providing recommendations for when to seek medical care if patients worsen or do not improve (i.e., a contingency plan) has been associated with higher visit satisfaction scores among patients who expected but were not prescribed antibiotics (66).
- Educate patients about the potential harms of antibiotic treatment. Potential harms might include common and sometimes serious side effects of antibiotics, including nausea, abdominal pain, diarrhea, C. difficile infection, allergic reactions, and other serious reactions. Parents of young children, in particular, want to be informed about possible adverse events associated with antibiotics (67). In addition, increasing evidence suggests antibiotic use in infancy and childhood is linked with allergic, infectious, and autoimmune diseases, likely through disturbing the microbiota (i.e., microorganisms within and on the human body) (68).
- Provide patient education materials. These materials might include information on appropriate antibiotic use, potential adverse drug events from antibiotics, and available resources regarding symptomatic relief for common infections. Educational materials on management of common infections are available online from CDC (http://www.cdc.gov/getsmart).
Outpatient clinic and health care system leaders can provide education to clinicians and ensure access to expertise by doing at least one of the following:
- Provide face-to-face educational training (academic detailing). This training can be provided by peers, colleagues, or opinion leaders, including other clinicians and pharmacists, and uses reinforcement techniques and peer-to-peer comparisons to facilitate changes in antibiotic prescribing practices (69–71).
- Provide continuing education activities for clinicians. Relevant continuing education activities include those that address appropriate antibiotic prescribing, adverse drug events, and communication strategies about appropriate antibiotic prescribing that can improve patient satisfaction. In particular, communications training in which clinicians were taught to assess patient expectations, discuss the risks and benefits of antibiotic treatment, provide recommendations for when to seek medical care if worsening or not improving (a contingency plan), and assess the patient’s understanding of the communicated information led to sustained decreases in inappropriate antibiotic prescribing (46,72).
- Ensure timely access to persons with expertise. Persons with expertise might include pharmacists or medical and surgical consultants who can assist clinicians in improving antibiotic prescribing for patients with conditions requiring specialty care. For example, in hospitals, pharmacists with infectious disease training have been effective and important members of antibiotic stewardship programs, and in hospital stewardship programs these types of pharmacists have been associated with improved patient outcomes and overall cost savings for the hospital (73). The expertise needed might differ among outpatient facilities and can be determined by each facility.
Future Directions
The Core Elements of Outpatient Antibiotic Stewardship provides a framework for improving antibiotic prescribing. Expanding horizons for outpatient health care delivery, such as outpatient parenteral antibiotic therapy, telemedicine and telehealth, and urgent care and retail clinics, might require unique stewardship approaches. Several studies have been published that show the benefit of antibiotic stewardship interventions in traditional primary care clinics (18,38,42). Additional implementation research is needed to determine which outpatient stewardship interventions work best in different outpatient settings, effective strategies to implement interventions, and sustainable approaches to outpatient stewardship.
Acute respiratory tract infections have been a focus of outpatient stewardship because these are the most common conditions leading to antibiotic treatment. However, additional efforts are needed to optimize stewardship efforts for other situations and syndromes that commonly lead to antibiotic use in the outpatient setting, including ambulatory procedures, dental prophylaxis, genitourinary infections, acne and other skin and soft tissue conditions, and chronic obstructive pulmonary disease.
Conclusion
Although the core elements provide a framework for outpatient antibiotic stewardship, implementing the elements requires a thoughtful and consistent effort to achieve desired outcomes. This includes developing strategies and preparing individuals, facilities, or organizations for change; developing and testing stewardship interventions; identifying and addressing barriers to change; and evaluating progress toward stated goals. Outpatient settings remain a crucial component of antibiotic stewardship in the United States. Establishing effective antibiotic stewardship interventions can protect patients and optimize clinical outcomes in outpatient health care settings.
Acknowledgments
Jonathan A. Finkelstein, MD, Boston Children’s Hospital, Harvard Medical School, Boston, Massachusetts; Jeffrey S. Gerber, MD, PhD, Children’s Hospital of Philadelphia, University of Pennsylvania Perelman School of Medicine, Philadelphia, Pennsylvania; Adam L. Hersh, MD, PhD, University of Utah, Salt Lake City, Salt Lake City, Utah; David Y. Hyun, MD, The Pew Charitable Trusts, Washington, DC; Jeffrey A. Linder, MD, Brigham and Women’s Hospital, Harvard Medical School, Boston, Massachusetts; Larissa S. May, MD, University of California—Davis, Sacramento, California; Daniel Merenstein, MD, Georgetown University Medical Center, Washington, DC; Katie J. Suda, PharmD, Department of Veterans Affairs, University of Illinois at Chicago, Chicago, Illinois; Kelly O’Neill, Austyn Dukes, and Rachel Robb, National Center for Emerging and Zoonotic Infectious Diseases, CDC, Atlanta, Georgia; Rachel Zetts, The Pew Charitable Trusts, Washington, DC.
Corresponding author: Katherine E. Fleming-Dutra, Division of Healthcare Quality Promotion, National Center for Emerging and Zoonotic Infectious Diseases, CDC. Telephone: 404-639-4243. E-mail: getsmart@cdc.gov.
References
- CDC. Antibiotic resistance threats in the United States, 2013 [Internet]. Atlanta, GA: US Department of Health and Human Services, CDC; 2013. http://www.cdc.gov/drugresistance/threat-report-2013/index.html
- CDC. Office-related antibiotic prescribing for persons aged ≤14 years—United States, 1993–1994 to 2007–2008. MMWR Morb Mortal Wkly Rep 2011;60:1153–6. PubMed
- Shapiro DJ, Hicks LA, Pavia AT, Hersh AL. Antibiotic prescribing for adults in ambulatory care in the USA, 2007–09. J Antimicrob Chemother 2014;69:234–40. CrossRef PubMed
- Gonzales R, Malone DC, Maselli JH, Sande MA. Excessive antibiotic use for acute respiratory infections in the United States. Clin Infect Dis 2001;33:757–62. CrossRef PubMed
- Fleming-Dutra KE, Hersh AL, Shapiro DJ, et al. Prevalence of inappropriate antibiotic prescriptions among U.S. ambulatory care visits, 2010–2011. JAMA 2016;315:1864–73. CrossRefPubMed
- Barlam TF, Cosgrove SE, Abbo LM, et al. Implementing an Antibiotic Stewardship Program: Guidelines by the Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America. Clin Infect Dis 2016;62:e51–77 CrossRef PubMed
- Seppälä H, Klaukka T, Vuopio-Varkila J, et al. ; Finnish Study Group for Antimicrobial Resistance. The effect of changes in the consumption of macrolide antibiotics on erythromycin resistance in group A streptococci in Finland. N Engl J Med 1997;337:441–6. CrossRef PubMed
- Suda KJ, Hicks LA, Roberts RM, Hunkler RJ, Danziger LH. A national evaluation of antibiotic expenditures by healthcare setting in the United States, 2009. J Antimicrob Chemother 2013;68:715–8. CrossRef PubMed
- Public Health England. English Surveillance Programme for Antimicrobial Utilisation and Resistance (ESPAUR): report 2014 [Internet]. London, England: Public Health England; 2014. https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/362374/ESPAUR_Report_2014__3_.pdf
- Public Health Agency of Sweden, National Veterinary Institute. Consumption of antibiotics and occurrence of antibiotic resistance in Sweden [Internet]. Swedres-Svarm 2014. Solna and Uppsala, Sweden: Public Health Agency of Sweden, National Veterinary Institute; 2015. Report No. ISSN 1650–6332. https://www.folkhalsomyndigheten.se/pagefiles/20281/Swedres-Svarm-2014-14027.pdf
- CDC. Outpatient antibiotic prescriptions—United States, 2013. Atlanta, GA: US Department of Health and Human Services, CDC; 2013. http://www.cdc.gov/getsmart/community/pdfs/annual-reportsummary_2013.pdf
- Hersh AL, Shapiro DJ, Pavia AT, Shah SS. Antibiotic prescribing in ambulatory pediatrics in the United States. Pediatrics 2011;128:1053–61. CrossRef PubMed
- Shehab N, Patel PR, Srinivasan A, Budnitz DS. Emergency department visits for antibiotic-associated adverse events. Clin Infect Dis 2008;47:735–43. CrossRef PubMed
- Kutty PK, Woods CW, Sena AC, et al. Risk factors for and estimated incidence of community-associated Clostridium difficile infection, North Carolina, USA. Emerg Infect Dis 2010;16:197–204.CrossRef PubMed
- Lessa FC, Mu Y, Bamberg WM, et al. Burden of Clostridium difficile infection in the United States. N Engl J Med 2015;372:825–34. CrossRef PubMed
- Wendt JM, Cohen JA, Mu Y, et al. Clostridium difficile infection among children across diverse U.S. geographic locations. Pediatrics 2014;133:651–8. CrossRef PubMed
- Dantes R, Mu Y, Hicks LA, et al. Association between outpatient antibiotic prescribing practices and community-associated Clostridium difficile infection. Open Forum Infect Dis 2015;2:ofv113.http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=26509182&dopt=Abstract CrossRef PubMed
- Meeker D, Knight TK, Friedberg MW, et al. Nudging guideline-concordant antibiotic prescribing: a randomized clinical trial. JAMA Intern Med 2014;174:425–31. CrossRef PubMed
- Meeker D, Linder JA, Fox CR, et al. Effect of behavioral interventions on inappropriate antibiotic prescribing among primary care practices: a randomized clinical trial. JAMA 2016;315:562–70.CrossRef PubMed
- Gerber JS, Prasad PA, Fiks AG, et al. Effect of an outpatient antimicrobial stewardship intervention on broad-spectrum antibiotic prescribing by primary care pediatricians: a randomized trial. JAMA 2013;309:2345–52. CrossRef PubMed
- CDC. Core elements of hospital antibiotic stewardship programs [Internet]. Atlanta, GA: US Department of Health and Human Services, CDC; 2014. http://www.cdc.gov/getsmart/healthcare/implementation/core-elements.html.
- Pollack LA, Srinivasan A. Core elements of hospital antibiotic stewardship programs from the Centers for Disease Control and Prevention. Clin Infect Dis 2014;59(Suppl 3):S97–100.CrossRef PubMed
- CDC. Core elements of antibiotic stewardship for nursing homes [Internet]. Atlanta, GA: US Department of Health and Human Services, CDC; 2014. http://www.cdc.gov/longtermcare/prevention/antibiotic-stewardship.html.
- Drekonja DM, Filice GA, Greer N, et al. Antimicrobial stewardship in outpatient settings: a systematic review. Infect Control Hosp Epidemiol 2015;36:142–52. CrossRef PubMed
- McDonagh M, Peterson K, Winthrop K, Cantor A, Holzhammer B, Buckley DI. Improving antibiotic prescribing for uncomplicated acute respiratory tract infections. AHRQ Comparative Effectiveness Reviews 2016. PubMed
- Ranji SR, Steinman MA, Shojania KG, Gonzales R. Interventions to reduce unnecessary antibiotic prescribing: a systematic review and quantitative analysis. Med Care 2008;46:847–62.CrossRef PubMed
- Arnold SR, Straus SE. Interventions to improve antibiotic prescribing practices in ambulatory care. Cochrane Database Syst Rev 2005;4:CD003539. PubMed
- van der Velden AW, Pijpers EJ, Kuyvenhoven MM, Tonkin-Crine SK, Little P, Verheij TJ. Effectiveness of physician-targeted interventions to improve antibiotic use for respiratory tract infections. Br J Gen Pract 2012;62:801–7. CrossRef PubMed
- Pollack LA, van Santen KL, Weiner LM, Dudeck MA, Edwards JR, Srinivasan A. Antibiotic stewardship programs in U.S. acute care hospitals: findings from the 2014 National Healthcare Safety Network Annual Hospital Survey. Clin Infect Dis 2016;63:443–9. CrossRef PubMed
- Chow AW, Benninger MS, Brook I, et al. Infectious Diseases Society of America. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis 2012;54:e72–112. CrossRef PubMed
- Gupta K, Hooton TM, Naber KG, et al. ; Infectious Diseases Society of America; European Society for Microbiology and Infectious Diseases. International clinical practice guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis in women: a 2010 update by the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases. Clin Infect Dis 2011;52:e103–20. CrossRef PubMed
- Lieberthal AS, Carroll AE, Chonmaitree T, et al. The diagnosis and management of acute otitis media. Pediatrics 2013;131:e964–99. CrossRef PubMed
- Mandell LA, Wunderink RG, Anzueto A, et al. ; Infectious Diseases Society of America; American Thoracic Society. Infectious Diseases Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clin Infect Dis 2007;44(Suppl 2):S27–72. CrossRef PubMed
- Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis 2012;55:1279–82. CrossRef PubMed
- Wald ER, Applegate KE, Bordley C, et al. American Academy of Pediatrics. Clinical practice guideline for the diagnosis and management of acute bacterial sinusitis in children aged 1 to 18 years. Pediatrics 2013;132:e262–80. CrossRef PubMed
- Little P, Moore M, Kelly J, et al. PIPS Investigators. Delayed antibiotic prescribing strategies for respiratory tract infections in primary care: pragmatic, factorial, randomised controlled trial. BMJ 2014;348:g1606. CrossRef PubMed
- Little P, Rumsby K, Kelly J, et al. Information leaflet and antibiotic prescribing strategies for acute lower respiratory tract infection: a randomized controlled trial. JAMA 2005;293:3029–35.CrossRef PubMed
- de la Poza Abad M, Mas Dalmau G, Moreno Bakedano M, et al. Delayed Antibiotic Prescription (DAP) Group. Prescription strategies in acute uncomplicated respiratory infections: a randomized clinical trial. JAMA Intern Med 2016;176:21–9. CrossRef PubMed
- Chao JH, Kunkov S, Reyes LB, Lichten S, Crain EF. Comparison of two approaches to observation therapy for acute otitis media in the emergency department. Pediatrics 2008;121:e1352–6.CrossRef PubMed
- Francis NA, Gillespie D, Nuttall J, et al. Delayed antibiotic prescribing and associated antibiotic consumption in adults with acute cough. Br J Gen Pract 2012;62:e639–46. CrossRefPubMed
- McCormick DP, Chonmaitree T, Pittman C, et al. Nonsevere acute otitis media: a clinical trial comparing outcomes of watchful waiting versus immediate antibiotic treatment. Pediatrics 2005;115:1455–65. CrossRef PubMed
- Siegel RM, Kiely M, Bien JP, et al. Treatment of otitis media with observation and a safety-net antibiotic prescription. Pediatrics 2003;112:527–31. CrossRef PubMed
- Spiro DM, Tay KY, Arnold DH, Dziura JD, Baker MD, Shapiro ED. Wait-and-see prescription for the treatment of acute otitis media: a randomized controlled trial. JAMA 2006;296:1235–41.CrossRef PubMed
- Rosenfeld RM, Piccirillo JF, Chandrasekhar SS, et al. Clinical practice guideline (update): Adult Sinusitis Executive Summary. Otolaryngol Head Neck Surg 2015;152:598–609. CrossRefPubMed
- Little P, Stuart B, Francis N, et al. GRACE consortium. Effects of internet-based training on antibiotic prescribing rates for acute respiratory-tract infections: a multinational, cluster, randomised, factorial, controlled trial. Lancet 2013;382:1175–82. CrossRef PubMed
- Cals JW, de Bock L, Beckers PJ, et al. Enhanced communication skills and C-reactive protein point-of-care testing for respiratory tract infection: 3.5-year follow-up of a cluster randomized trial. Ann Fam Med 2013;11:157–64. CrossRef PubMed
- McGinn TG, McCullagh L, Kannry J, et al. Efficacy of an evidence-based clinical decision support in primary care practices: a randomized clinical trial. JAMA Intern Med 2013;173:1584–91.CrossRef PubMed
- Jenkins TC, Irwin A, Coombs L, et al. Effects of clinical pathways for common outpatient infections on antibiotic prescribing. Am J Med 2013;126:327–335.e12. CrossRef PubMed
- Gonzales R, Anderer T, McCulloch CE, et al. A cluster randomized trial of decision support strategies for reducing antibiotic use in acute bronchitis. JAMA Intern Med 2013;173:267–73.CrossRef PubMed
- Rattinger GB, Mullins CD, Zuckerman IH, et al. A sustainable strategy to prevent misuse of antibiotics for acute respiratory infections. PLoS One 2012;7:e51147. CrossRef PubMed
- Linder JA, Schnipper JL, Tsurikova R, et al. Documentation-based clinical decision support to improve antibiotic prescribing for acute respiratory infections in primary care: a cluster randomised controlled trial. Inform Prim Care 2009;17:231–40. PubMed
- Forrest CB, Fiks AG, Bailey LC, et al. Improving adherence to otitis media guidelines with clinical decision support and physician feedback. Pediatrics 2013;131:e1071–81 . CrossRefPubMed
- Harper R, Temkin T, Bhargava R. Optimizing the use of telephone nursing advice for upper respiratory infection symptoms. Am J Manag Care 2015;21:264–70. PubMed
- Metlay JP, Camargo CA , MacKenzie T, et al. IMPAACT Investigators. Cluster-randomized trial to improve antibiotic use for adults with acute respiratory infections treated in emergency departments. Ann Emerg Med 2007;50:221–30. CrossRef PubMed
- Finkelstein JA, Huang SS, Kleinman K, et al. Impact of a 16-community trial to promote judicious antibiotic use in Massachusetts. Pediatrics 2008;121:e15–23. CrossRef PubMed
- Butler CC, Simpson SA, Dunstan F, et al. Effectiveness of multifaceted educational programme to reduce antibiotic dispensing in primary care: practice based randomised controlled trial. BMJ 2012;344:d8173. CrossRef PubMed
- Dempsey PP, Businger AC, Whaley LE, Gagne JJ, Linder JA. Primary care clinicians’ perceptions about antibiotic prescribing for acute bronchitis: a qualitative study. BMC Fam Pract 2014;15:194. CrossRef PubMed
- Hallsworth M, Chadborn T, Sallis A, et al. Provision of social norm feedback to high prescribers of antibiotics in general practice: a pragmatic national randomised controlled trial. Lancet 2016;387:1743–52. CrossRef PubMed
- Harris AM, Hicks LA, Qaseem A; High Value Care Task Force of the American College of Physicians and for the Centers for Disease Control and Prevention. Appropriate antibiotic use for acute respiratory tract infection in adults: advice for high-value care from the American College of Physicians and the Centers for Disease Control and Prevention. Ann Intern Med 2016;164:425–34. CrossRef PubMed
- Hersh AL, Jackson MA, Hicks LA; American Academy of Pediatrics Committee on Infectious Diseases. Principles of judicious antibiotic prescribing for upper respiratory tract infections in pediatrics. Pediatrics 2013;132:1146–54 . CrossRef PubMed
- The White House. National action plan for combating antibiotic-resistant bacteria [Internet]. Washington, DC: The White House; 2015. https://www.whitehouse.gov/sites/default/files/docs/national_action_plan_for_combating_antibotic-resistant_bacteria.pdf
- National Committee for Quality Assurance. HEDIS & performance measurement [Internet]. Washington, DC: National Committee for Quality Assurance; 2016. http://www.ncqa.org/hedis-quality-measurement.
- Harris RH, MacKenzie TD, Leeman-Castillo B, et al. Optimizing antibiotic prescribing for acute respiratory tract infections in an urban urgent care clinic. J Gen Intern Med 2003;18:326–34.CrossRef PubMed
- Juzych NS, Banerjee M, Essenmacher L, Lerner SA. Improvements in antimicrobial prescribing for treatment of upper respiratory tract infections through provider education. J Gen Intern Med 2005;20:901–5.http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16191135&dopt=Abstract CrossRef PubMed
- Mangione-Smith R, Zhou C, Robinson JD, Taylor JA, Elliott MN, Heritage J. Communication practices and antibiotic use for acute respiratory tract infections in children. Ann Fam Med 2015;13:221–7. CrossRef PubMed
- Mangione-Smith R, McGlynn EA, Elliott MN, McDonald L, Franz CE, Kravitz RL. Parent expectations for antibiotics, physician-parent communication, and satisfaction. Arch Pediatr Adolesc Med 2001;155:800–6. CrossRef PubMed
- Roberts RM, Albert AP, Johnson DD, Hicks LA. Can improving knowledge of antibiotic-associated adverse drug events reduce parent and patient demand for antibiotics? Health Serv Res Manag Epidemiol 2015;2. CrossRef
- Vangay P, Ward T, Gerber JS, Knights D. Antibiotics, pediatric dysbiosis, and disease. Cell Host Microbe 2015;17:553–64. CrossRef PubMed
- Gjelstad S, Høye S, Straand J, Brekke M, Dalen I, Lindbæk M. Improving antibiotic prescribing in acute respiratory tract infections: cluster randomised trial from Norwegian general practice (prescription peer academic detailing (Rx-PAD) study). BMJ 2013;347:f4403. CrossRef PubMed
- Solomon DH, Van Houten L, Glynn RJ, et al. Academic detailing to improve use of broad-spectrum antibiotics at an academic medical center. Arch Intern Med 2001;161:1897–902. CrossRefPubMed
- Soumerai SB, Avorn J. Principles of educational outreach (‘academic detailing’) to improve clinical decision making. JAMA 1990;263:549–56. CrossRef PubMed
- Cals JWL, Scheppers NAM, Hopstaken RM, et al. Evidence based management of acute bronchitis; sustained competence of enhanced communication skills acquisition in general practice. Patient Educ Couns 2007;68:270–8. CrossRef PubMed
- Yu K, Rho J, Morcos M, et al. Evaluation of dedicated infectious diseases pharmacists on antimicrobial stewardship teams. Am J Health Syst Pharm 2014;71:1019–28. CrossRef PubMed



































No hay comentarios:
Publicar un comentario